 Central Hypotonia
Central Hypotonia
- Section I: Evidence Summary
- Section II: Selected Published Evidence
- Section III: Practical Tools
- Section IV: Acknowledgments
- Language/
Translations - Feedback/
Comments
Section I: Evidence Summary Printer Friendly Version
A. Definitions
Hypotonia can be defined as abnormally low muscle tone, or reduced resistance to passive, relatively rapid movement. The imprecision of the definition reflects the lack of psychometric properties and reliability of assessments for hypotonia, therefore only clinical definitions currently in use by neurology specialists will be used in this pathway. Other terms for hypotonia include, but are not limited to, central hypotonia, floppy baby syndrome, benign congenital hypotonia, and neonatal hypotonia.
Hypotonia may originate from disturbances in the physiology of central or peripheral nervous systems or of the end organs themselves (muscles and muscle groups). The current pathway will only address children whose hypotonia is centrally-mediated and will exclude those whose hypotonia can be attributed conclusively to peripheral causes. Spinal Muscular Atrophy (SMA) is not included within the definition of centrally mediated hypotonia. Centrally-mediated hypotonia will be further referred to in this document as “central hypotonia” in the interest of simplicity. Specific etiologies of central hypotonia include brain insults and malformations, as well as genetic, metabolic, traumatic, anatomical, or idiopathic causes of central neural dysfunction.
Central hypotonia may be generalized and affect the limbs, trunk and neck or may be localized such that specific areas of the body are predominantly hypotonic with others having normal or hypertonic characteristics. Hypotonia is often seen in combination with muscle weakness. In the case of perinatal insults to white matter tracts, such as in encephalopathy of prematurity and neonatal encephalopathy, central hypotonia can evolve over the course of the first few years of life and progress to hypertonia. In addition, central hypotonia can co-exist with abnormalities of movement (such as ataxia or dyskinesia) or sensation (dysethesias, paresthesias).
B. Why is Therapeutic Assessment and Intervention Important for Children (age 0-6 years) with Central Hypotonia?
Infants and young children with diagnoses of Down syndrome (DS), Cerebral Palsy (CP), and/or developmental delay (DD) often present with low muscle tone that can influence their gross motor development. Other children presenting to therapists may have no established diagnoses.
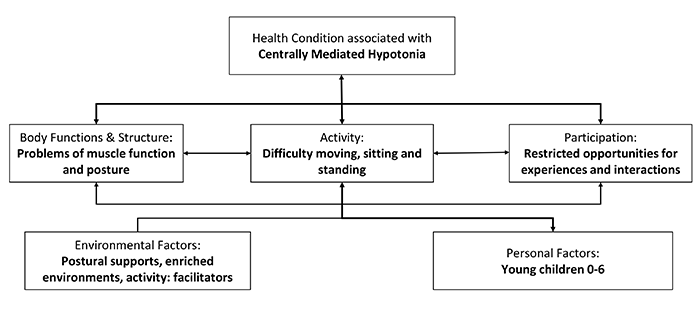
- Central hypotonia can impede motor function through decreased joint stability, joint hypermobility, weakness, and/or decreased activity and endurance.
- Impaired motor function can be associated with reduced developmental experiences in turn altering typical progression of gross and fine motor abilities.
- Central hypotonia can interfere with ability to attain positions and acquisition of developmental milestones.
- Hypotonic postures can interfere with functional activities such as reaching, sitting, standing and crawling/walking, which can lead to participation restrictions.
- Central hypotonia, in combination with muscle weakness, can interfere with sleep by limiting ability to change position during rest: this can contribute to discomfort and poor sleep quality.
- Central hypotonia can result in reflux and/or constipation due to abnormalities in coordination of voluntary and involuntary muscle function.
- Hypotonic postures and low muscle activity can create challenges for care-giving and participation in daily life activities.
- Children with central hypotonia can have drooling and feeding problems (e.g. chewing or swallowing).
C. Target Population
Children from birth to six years-of-age with central hypotonia and gross motor delays that limit activity and participation.
D. Target Clinical Providers
Therapists/Early Interventionists caring for children from birth to six years-of-age with central hypotonia and their families.
E. Assessment
If the child has not already been seen for a diagnostic work-up, referral to a neurologist, geneticist and/or developmental medical specialist is always recommended. During the therapy assessment, determine the impact of the hypotonia on function, activity limitations and participation restrictions, pain/comfort (including sleep), care-giving and whether management is required. Assess whether the clinical presentation is consistent with infants at “high risk of CP” (see Early Detection Guidelines, JAMA Pediatrics Novak et al. 2017).
Therapy Assessment: Children with hypotonia may have delays in motor development. It is recommended that therapists use valid and reliable measures of motor abilities. As there are no established evidence-based approaches to measure hypotonia, and as the focus of therapy should be on improved functioning, we recommend the following: use motor function assessments with good psychometric properties for infants at high risk for motor delays and neuromotor problems such as: the Hammersmith Infant Neurological Examination (HINE, 3 to 24 months), the Test of Infant Motor Performance (TIMP, term to 3 months), Peabody Developmental Motor Scales (PDMS), Development Assessment of Young Children (DAYC-2) Motor Scale, the Alberta Infant Motor Scale (AIMS, 0-18 months), Brigance III, etc. (See Early Detection Guidelines for CP, JAMA Pediatrics Novak et al., 2017). A broader perspective on promoting child development is offered by the ‘F words in childhood disability’ (Rosenbaum & Gorter, 2012)
Goal Setting: Use valid and reliable outcome measures outcomes such as Canadian Occupational Performance Measure (COPM), Goal Attainment Scaling (GAS) (see Section III for further details).
F. Management
Most of the interventions in the Central Hypotonia Care Pathway have low or very low levels of evidence (based on GRADE ratings).
Developmental Strategies: strategies used by physiotherapists (PTs), occupational therapists (OTs) and early interventionists are considered cornerstones in the management of central hypotonia. General principles include:
- ensure therapy is goal-directed and promotes function and participation in daily activities/routines.
- ensure all motor interventions are child active.
- activities should be child-initiated and child-directed.
- activities should be caregiver delivered when possible.
- optimize seating and upright positioning with good stability/support as early as possible (providing opportunities for reach/grasp and manipulation to learn through play).
- avoid extreme positions (e.g. frog-legged (hip/knee flexion with abduction)) and strive for symmetry.
- consider orthoses and splints to increase foot stability in stance and weight bearing.
- encourage early mobility using various typical, adapted and specialized equipment.
- coach parents to integrate therapeutic interventions for hypotonia into daily life and routines.
- avoid passive interventions in which the therapist performs the work for the child and/or the child is not moving actively (reduce hands-on time and overt assistance, allow for infant-initiated activities).
- avoid interventions for which there is no evidence and/or a risk of negative outcomes (see section II for further details).
- ensure screening for other health concerns and comorbidities including; with vision, hearing, feeding, reflux, and communication.
G. Therapeutic Recommendations
(for details on each intervention including potential risks, see the evidence summary in Section II):
- Tummy Time activities (during supervised play, when a child is awake), for multiple short sessions per day, may promote motor development in young children with central hypotonia.
- Active motor abilities should be promoted in sitting, standing and for mobility.
- Infant massage may be used to promote mother-infant bonding and sleep.
- Treadmill training may be used from 10 months onward, to promote early onset of stepping, walking and improve gait characteristics in children with central hypotonia.
- Orthotics may be used to support foot alignment and improve gait characteristics for ambulatory children with central hypotonia; in pre-ambulatory children, expert opinion recommends trial and/or use of orthoses when ankle instability prevents age appropriate exploration.
- Adaptive equipment may increase activity and participation: e.g. adaptive seating; compression garments, walker/gait trainer; stander; and power mobility devices.
- Postural management programs facilitate age appropriate activity and participation in natural routines (i.e. activities in lying, supported sitting, standing). Postural management programs should reduce time spent in asymmetrical lying postures and frog-legged positions.
- Hip surveillance to monitor hip displacement can enable referral for early intervention to prevent hip subluxation and dislocation, which is known to occur in children with central hypotonia (see AACPDM Hip Surveillance Care Pathway for information on surveillance in children with cerebral palsy).
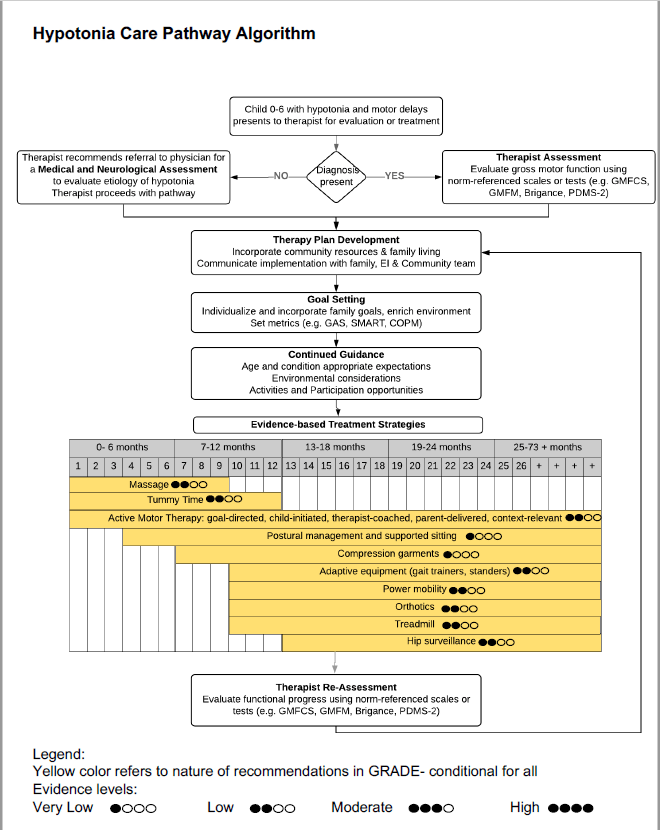
Central Hypotonia Evidence for Interventions - GRADE ratings
Section II: Selected Published Evidence
Click on the links for free full text.
- Paleg G, Romness M, Livingstone R. Interventions to improve sensory and motor outcomes for young children with central hypotonia: A systematic review. J Pediatr Rehabil Med. 2018;11(1):57-70.
- Valentin-Gudiol M, Bagur-Calafat C, Girabent-Farres M, Hadders-Algra M, Mattern-Baxter K, Angulo-Barroso R. Treadmill interventions with partial body weight support in children under six years of age at risk of neuromotor delay: a report of a Cochrane systematic review and meta-analysis. Eur J Phys Rehabil Med 2013;49(1):67-91.
- Weber A, Martin K. Efficacy of Orthoses for Children With Hypotonia: A Systematic Review. Pediatr Phys Ther. 2014;26:38-47
Central Hypotonia Evidence for Interventions - GRADE ratings
Section III: Practical Tools
Plain Language Summary

Helpful Key References
- Darrah J, O'Donnell M, Lam J, Story M, Wickenheiser D, Xu K, et al. Designing a Clinical Framework to Guide Gross Motor Intervention Decisions for Infants and Young Children With Hypotonia. Infants & Young Children. 2013;26(3):225-34.
- Novak I, Morgan C, Adde L, Blackman J, Boyd RN, Brunstrom-Hernandez J, et al. Early, Accurate Diagnosis and Early Intervention in Cerebral Palsy: Advances in Diagnosis and Treatment. JAMA pediatrics. 2017;171(9):897-907.
- Martin KS, Westcott S, Wrotniak BH. Diagnosis dialog for pediatric physical therapists: hypotonia, developmental coordination disorder, and pediatric obesity as examples. Pediatr Phys Ther. 2013;25(4):431-43.
- Martin K, Kaltenmark T, Lewallen A, Smith C, Yoshida A. Clinical characteristics of hypotonia: a survey of pediatric physical and occupational therapists. Pediatr Phys Ther. 2007;19(3):217-26.
- Martin K, Inman J, Kirschner A, Deming K, Gumbel R, Voelker L. Characteristics of hypotonia in children: a consensus opinion of pediatric occupational and physical therapists. Pediatr Phys Ther. 2005;17(4):275-82.
- Govender P, Joubert RWE. 'Toning' up hypotonia assessment: A proposal and critique. African journal of disability. 2016;5(1):231.
- Govender P, Joubert RWE. Evidence-Based Clinical Algorithm for Hypotonia Assessment: To Pardon the Errs. Occupational therapy international. 2018;2018:8967572.
- Glegg SM, Livingstone R, Montgomery I. Facilitating interprofessional evidence-based practice in paediatric rehabilitation: development, implementation and evaluation of an online toolkit for health professionals. Disabil Rehabil. 2016;38(4):391-9.
- Rosenbaum P, Gorter JW. The 'F-words' in childhood disability: I swear this is how we should think! Child Care Health Dev. 2012;38(4):457-63.
Practical Tools
 |
A. Hypotonia Wheel and Guide |
B. Clinical Assessment of Hypotonia Tools:
- HINE article
- HINE information and video
- Test of Infant Motor Performance Test (TIMP)
- Website on hypotonia
- CP Toolkit
C. Goal Setting Tools:
D. Diagnostic Algorithms:
Section IV: Acknowledgments
Stakeholder Consultation:
Three families with children aged between 3 months and 6 years-of-age with varying degrees of hypotonia reviewed the pathway and provided written feedback that was incorporated into the care pathway.
Expert Consensus Team:
| Name | Affiliation(s) and specialty | Location | Role |
|---|---|---|---|
| Ginny Paleg, PT, MPT, DScPT | Montgomery County Infants and Toddlers Program Physical Therapist |
Rockville, Maryland, USA | Team Leader, Author and Consensus Expert Author of Systematic Review |
| Roslyn Livingstone, MSc(RS) OT | Sunny Hill Health Centre for Children Occupational Therapist |
Vancouver, British Columbia, Canada | Author and Consensus Expert Author of Systematic Review |
| Elisabet Rodby-Bousquet, PT, PhD | Centre for Clinical Research, Uppsala University Associate Professor Lund University and Physical Therapist |
Västerås, Sweden | Author and Consensus Expert |
| Maureen Story, BSR PT/OT | Sunny Hill Health Centre for Children Occupational and Physical Therapist |
Vancouver, British Columbia, Canada | Co-Author of Hypotonia Tool Kit and Wheel and Consensus Expert |
| Nathalie L Maitre, MD, PhD | Nationwide Children’s Hospital Associate Professor of Pediatrics and Neonatologist | Columbus, Ohio, USA | Author and Consensus expert |
| Pragashne (Naidoo) Govender, PhD | School of Health Sciences, University of KwaZulu-Natal Associate Professor and Occupational Therapist |
Durban, South Africa | Consensus Expert |
| Mark Romness, MD | Department of Orthopedic Surgery University of Virginia Associate Professor and Pediatric Orthopedic Surgeon |
Charlottesville, VA, USA | Consensus Expert Author of Systematic Review |
| Christopher Lunsford, MD | Department of Orthopedic Surgery and Department of Pediatrics Duke University Pediatric Physiatrist |
Durham, NC, USA | Consensus Expert |
| Garey Noritz, MD | Nationwide Children’s Hospital Division Chief of the Complex Health Care Program Professor of Pediatrics and Ohio State University Developmental Pediatrician and Internist |
Columbus, OH, USA | Consensus Expert |
| Julia Looper, PT, PhD | University of Puget Sound Associate Professor of Physical Therapy and Physical Therapist |
Tacoma, WA, USA | Consensus Expert |
| Kathy Martin, PT, DHSc | University of Indianapolis Krannert School of Physical Therapy Professor, DPT Program Director and Physical Therapist |
Indianapolis, IN, USA | Consensus Expert |
| Lourdes Macias, PT, PhD, MSc | Universitat Internacional de Catalunya Early Intervention Public Department, President of the Spanish Pediatric Physical Therapy Association (SEFIP), Professor and Physical Therapist |
Barcelona, Spain | Consensus Expert |
| Sharon Eylon, MD | ALYN Rehabilitation Hospital for Children and Adolescents Head of Orthopedic Services Pediatric Orthopedic Surgeon |
Jerusalem, Israel | Consensus Expert |
Language/Translations
Spanish Version

Feedback/Comments
The American Academy for Cerebral Palsy and Developmental Medicine has developed care pathways to assist the busy clinician. Please submit any advice or constructive feedback to make this pathway more useful.
NOTE: Feedback will be directed to the AACPDM Care Pathway Taskforce to review and consider on a queue 6-month basis.


